Dr. Oscar John Ma on Using Ultrasound to Detect COVID-19

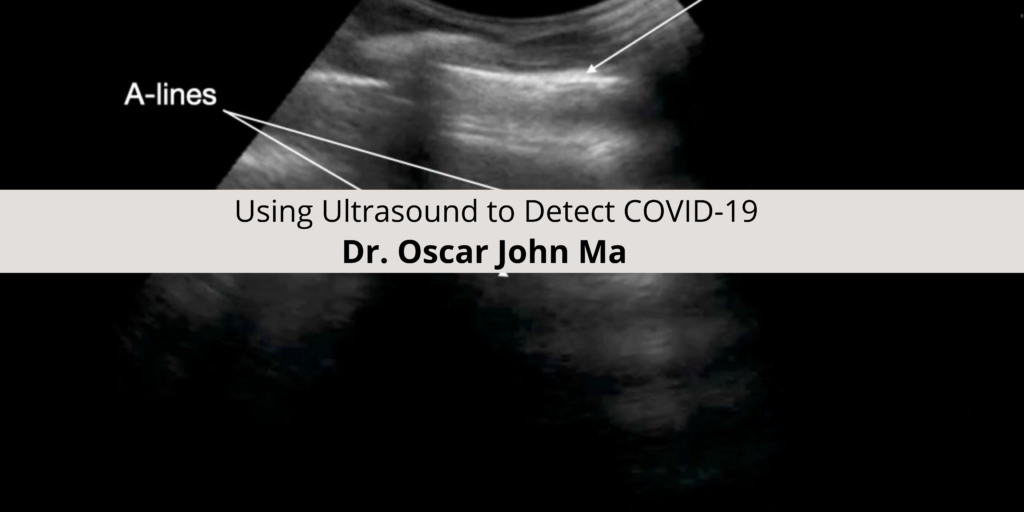
The COVID-19 pandemic has required medical providers to find innovative methods first to detect and then to assess the severity of the disease. In 2021, we now have rapid PCR and slower antibody testing for the virus. Assessing the severity of the disease, however, still remains a challenge.
As Dr. Oscar John Ma pointed out in the fourth edition of Ma and Mateer’s Emergency Ultrasound, point-of-care ultrasound proved to be a vital tool in diagnosing COVID-19 at the beginning of the pandemic, before other methods were widely available. Testing was either unavailable, or prohibitively expensive, or suffered an excessively long turnaround time for timely treatment of patients presenting COVID-19 symptoms. Emergency physicians found that computer tomography was beneficial for triaging patients, because patients may demonstrate radiologic findings before they present hallmark symptoms of the disease.
However, computed tomography presented its own challenges. CT scanning entailed additional exposures of technicians, transport staff, nurses, and physicians to the pathogen. The American College of Radiology advised against the diagnostic use of computed tomography both in the ER and for hospitalized patients.
Fortunately, Dr. Ma points out, point-of-care ultrasound of the lung has proven comparable to computed tomography and chest radiography for detection of pleural and parenchymal pathology. Historically, ultrasound was an important tool for rapid diagnosis and assessment of pulmonary status of patients in the 2013 H7N9 (avian flu) epidemic. Point-of-care ultrasonography was used for assessment of pulmonary function in Ebola patients. Similarly, point-of-care lung ultrasound has proven useful in earlier detection of pulmonary infection with the coronavirus. The absence of radiation exposure and ease of sterilization of equipment has made ultrasound a vital diagnostic tool in hospitals suffering stress on their resources.
Just how big a difference can the use of ultrasound make in stretching limited hospital resources?
Dr. Oscar John Ma points out that:
The cost of an ultrasound machine varies from $30,000 to more than $150,000, prohibiting access to resource-limited clinics and hospitals. Transportation of these sizable devices adds to their acquisition cost. Portable ultrasound units are available for $2000 to $2500.
Any diagnostic machines must be thoroughly sterilized after each use. A single hand-held probe is easy to sterilize, while considerable effort is required to sterilize a CT scanner.
But the benefits of point-of-care lung ultrasound are not limited to diagnosis. This tool can also supplant radiography and computed tomography for monitoring response to therapy. It is not necessary to transport critically ill patients to the radiology department to confirm or disconfirm response to treatment.
Ultrasound, Dr. Oscar John Ma, asserts, plays a vital role in providing urgent care. Point-of-care ultrasound is an accurate, reliable, and cost-effective diagnostic tool for medical providers.
